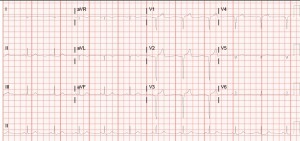
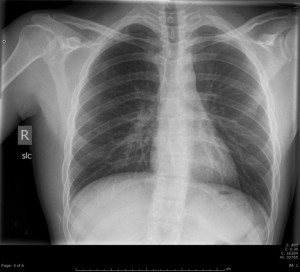
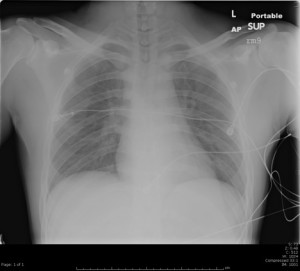
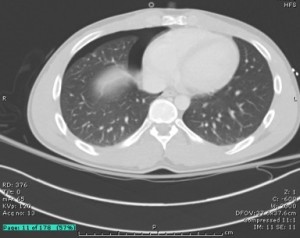
Recently saw at case at ULH (Not mine but posted with permission from resident involved) of a young female (18-20yo) flown from OSH for copperhead bite to L foot. Pt had been hiking in the woods with her boyfriend when she felt a stabbing sensation on her foot, looked down and there was a snake. Pt took a picture of it – sure enough it was a copperhead. Labs at OSH wnl, sent to ULH for concern for possible need for antivenin. I realized – being an urban trauma center – we don’t see a lot of snake bites. If you’re from the area, you may not be familiar with our venomous critters.
There are four species of venomous snakes in KY, all pit vipers (triangular heads, heavy bodies, cat-like pupils) – fw.ky.gov
1. Copperhead – extremely common throughout the state, most common envenomation, mildest venom of the four. (As an acquaintance of mine, Jim Harrison of East KY Venom Extraction lab used to say – no recorded history of death from copperhead envenomation in KY history
2. Timber Rattlesnake – found throughout state, potent venom, relatively docile. Dark coloration, have a rattle (obviously)
3. Pygmy Rattlesnake – found in extreme Western KY. Also have a rattle, potent venom
4. Cottonmouth – found in Western KY, potent venom, can be aggressive. Can be mistaken for Eastern Water Snake (common, non-venomous, aggressive water-dwelling snake found throughout KY)
Best identification – hopefully someone took a picture – otherwise, one to two small puncture wounds with increasing swelling and pain are good signs of envenomation. However, approximately 25% of viper envenomations can be dry bites – where snake gives a warning bite, injects no venom.
Signs and Symptoms of snake bite:
Venomous snakes in KY typically have venoms containing cytotoxins and hemotoxins – they break down tissue and can act on coagulations factors
-puncture wounds (usually paired, can be one)
-erythema and swelling
-intense pain at site and increasing proximally
-systemic symptoms can include nausea, vomiting, abdominal pain, vertigo. Altered mental status and hypotension can present as well
First Aid if bitten:
-Walk slowly – increased activity increases circulation of venom
-Elevate affected part: most bites are on distal extremities: feet, hands. More serious complications are associated with bites involving trunk, neck, face
-Wash with soap and water
DO NOT:
-Apply a tourniquet
-Attempt to suck venom from wound
-Apply ice to wound
Medical Work-up for known or suspected envenomation
-ABCs (always the first step)
-Good H&P – observe amount of swelling, movement of affected area. Mark swelling and erythema with marker to observe for progression
-CBC
-Comp
-Coags
-Total CK
-Fibrinogen
-U/A – to look for myoglobinuria
-Consider ABG and lactic acid if signs of systemic toxicity
-Xray to r/o retained teeth
Severe complications
-Rhabdomyolysis – from muscle breakdown from venom
-Compartment syndrome – cannot be diagnosed on clinical exam alone. Venom can cause tingling and paresthesias. If concerned, consult your surgeon
-Thrombocytopenia and coagulopathy – caused by thrombin-like molecules in venom. Treated with antivenom
-Systemic toxicity – can be life-threatening
Treatment:
-Update Tdap if indicated
-Pain control, elevation
-Antivenom if indicated
Antivenin: Always contact your toxicologist prior to giving
-Recommended for moderate to severe envenomations
(http://www.uptodate.com.echo.louisville.edu/contents/image?imageKey=EM%2F53948&topicKey=EM%2F6595&rank=2%7E39&source=see_link&search=snake+bite&utdPopup=true)
-Dosing: Moderate envenomation – 4 to 6 vials (1g each) over 60 min with repeat dose as needed
Severe envenomation – 6 to 9 vials over 60min with repeat dose prn
-Contraindications: papaya allergy (contains enzyme papain)
-Stop if signs of anaphylaxis
Disposition
-Requires antivenom – admission. Complications can include compartment syndrome, delayed coagulopathy (up to 48hrs). May need redosing of antivenom
-Mild envenomation or no symptoms – can be discharged home if pain controlled and no signs of toxicity at 8-12hrs s/p bite. If bitten by rattlesnake or cottonmouth, recommend CBC, PT, fibrinogen at 2-3d and 5-6d after initial bite
![Room9er ["Room Niner"]:](https://room9er.com/wp-content/uploads/2020/03/cropped-Screen-Shot-2020-03-08-at-3.16.16-PM.png)