Abnormal vital signs are always something to keep an eye on. Always important to explain it in documentation, but keep an eye on the trend throughout your shift as it’s one piece of information that might tip you off that something else may going on. Try to resolve the vital signs prior to discharge, looks better from a chart buffing standpoint, but also an indication that you have corrected the original problem. And if you can’t, again explain it, or just don’t discharge the patient. You will never be 100% in this job, and your initial impression could be flat out wrong, so putting in little safeguards to protect yourself, from well yourself, can help you not miss things.
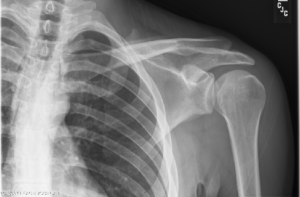
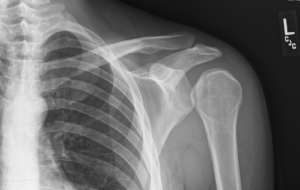
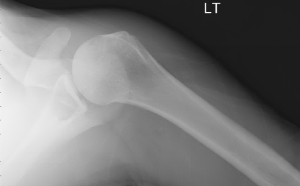
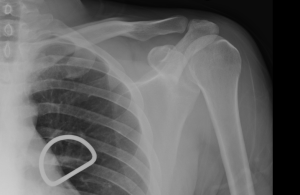
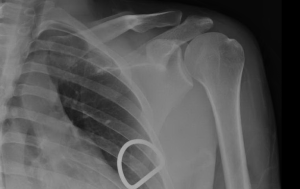
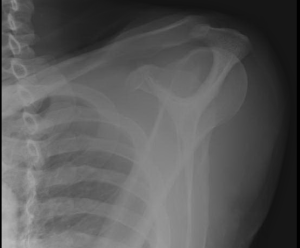
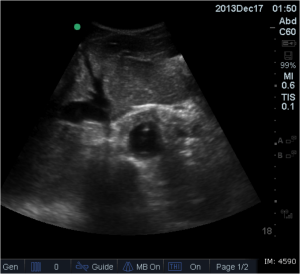
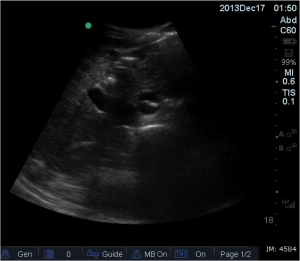
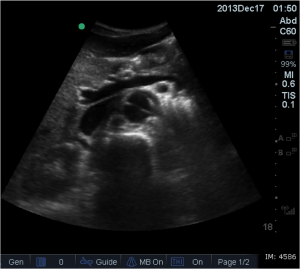
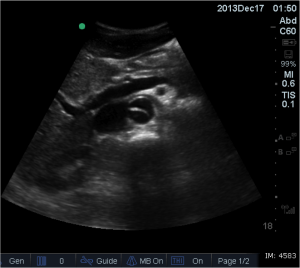
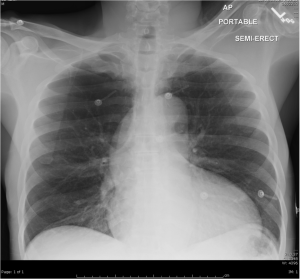
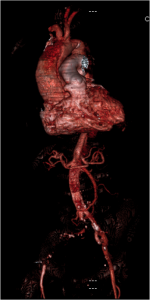
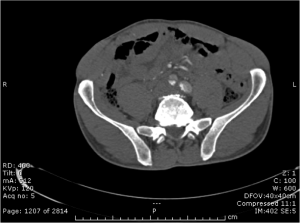
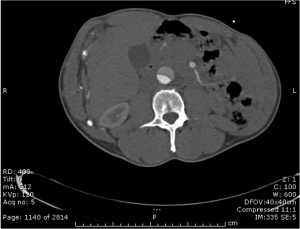
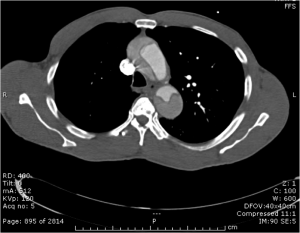
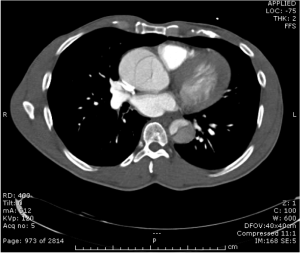
Quick case…..47 y/o M, history of 75% TBSA burns, active c-diff, PNA presents to the ED for low Hgb. Had Hgb of 7 at NH, 6.4 when checked here. Was just discharged recently from our ER (by myself, VSS at d/c) with new blisters on L scalp, Hgb was 7.3 at that time, 7-7.8 on prior visits. Wbc count: 11.8. Chronic indwelling foley. Urine dip: blood/wbcs/bacteria, neg leuk esterase/nitrite, already on levaquin for known PNA as well. Sinus tach to 120s. Received transfusion x2 units and initial plan was d/c back to nursing home per initial resident. Checked out to 2nd resident (myself) HR remained tachy to 120. Medicine consulted for admission. He was Afebrile. Blood cultures/urine cultures/ sputum cultured ordered as he did have an elevated WBC. Broad spectrum abx ordered. Rectal temp ordered x2, which were both normal. Medicine consulted for low hgb, sinus tach, and they cancelled cultures and abx, felt it was due to anemia although it did not improve with 2 unit transfusion (they are not always right). Planned for anemia work up and obs.
The patient admitted to the hospital and transfused. Hgb trended down again and patient required transfusion again on 9/26. Neg hemoccult/GI bleeding. Anemia work up not completed, but appeared to likely be of chronic disease vs iron deficiency. Patient became febrile on 9/23, BP dropped (that’s 3 days later…..) Started on broad spectrum abx, pan cultured. Urine grew acinetobacter. Blood cultures neg/c-diff negative. Hypotension was not responsive to fluids. Palliative consulted, patient and family elected to be comfort care. Made DNR. Comfort measures in place, was to be discharged to hospice. Patient subsequently expired prior to discharge on 10/4, etiology believed to be sepsis.
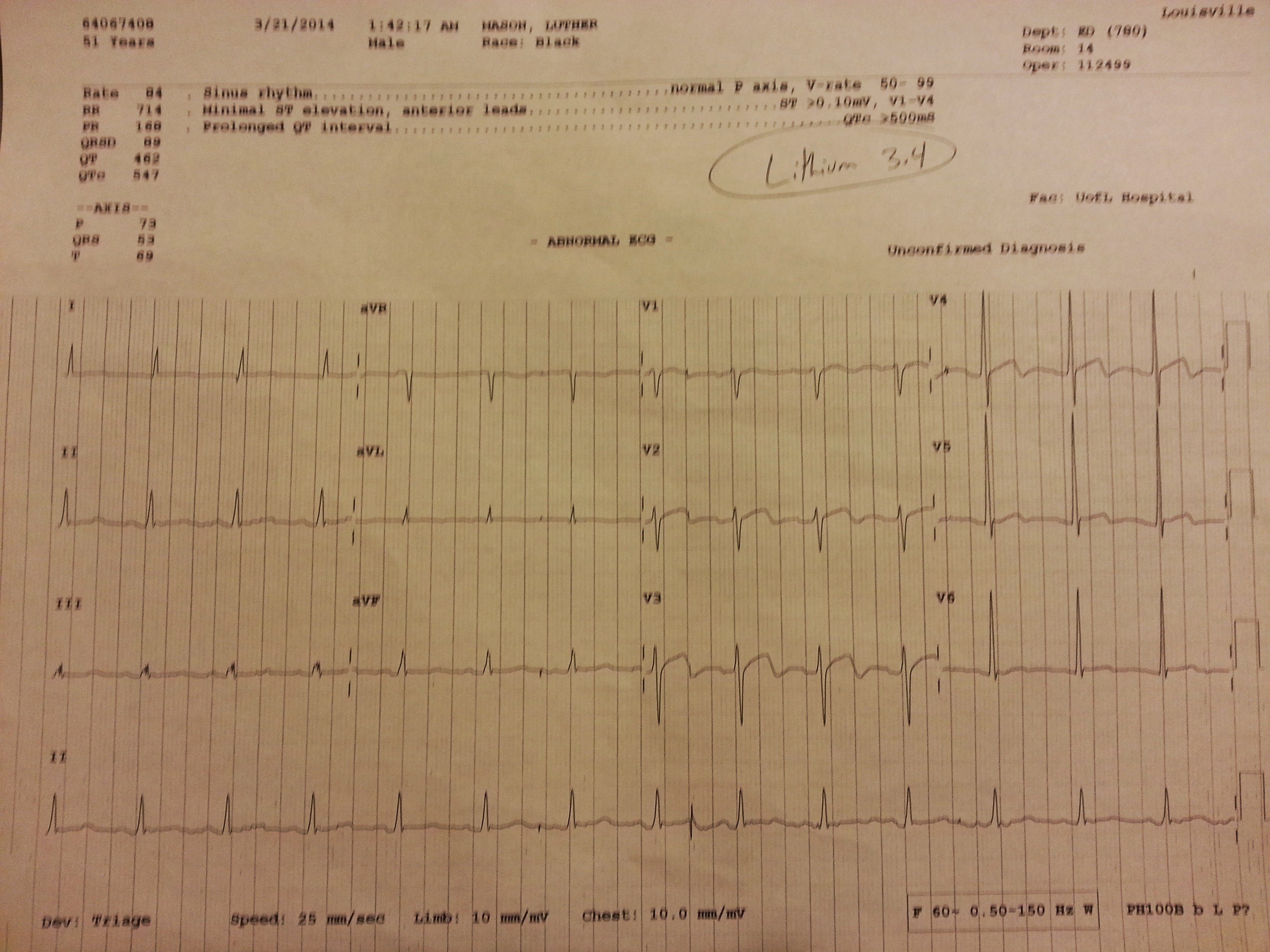
This patient had obviously a lot going on. Sinus tach could’ve been from anemia, pain, sepsis, stress, anxiety, etc. The initial thought it was due to anemia. but if this was true, it should come down with fluids and/or blood? Or at least partially respond? But it didn’t budge. He’s obviously had a long in-house history with the history of the burns so he was set up for a resistant bug, odd presentation. And honestly when we start seeing PNA + UTI we should start leaning towards sepsis from 1 agent with seeding, rather than a PNA and a UTI as two different infections going on. But in the end when he was checked out to me and the HR hadn’t budged, that was the tip off that something else was going on.
To expand on this as you can see things weren’t handled as they should’ve been initially. I see some people use the medicine service as a consultant. Which I thoroughly don’t believe in. They practice essentially the same thing as us, except less broad, more in depth, and a hell of a lot more boring (yes offense). When we talk to NES or neurology, or OB, or any of the other sub-specialties we are generally looking for guidance and information about a practice that is beyond our skills, beyond just basic medicine. And they have texts/papers/experience/OR time that allows them to function as a consultant and specialist in their area (especially the surgical services!).
But the medicine service is not all that different from what we do. When we call them, it shouldn’t be, “come see if this guy is ok for discharge.” We know which ones are and aren’t. And if you don’t, read more, use 5-minute EM consult, follow up on the patients you admit, so you can get a better understanding of what happens beyond the ED. You might not know the entire algorithm for hyponatremia and what work up they exactly do, but you should know when to admit one and how to emergently treat it. Or when to transition from insulin gtt to metformin, but you know when the glucose is too high to dispo home. Etc etc……. In their defense, sometimes we call them with patients that can theoretically be managed at home to begin with, but don’t fool yourself into thinking they know exactly what can go home and what can stay, and that they are the almighty, all-knowing doctor (case in point above.) They are residents too, and they don’t have an attending looking into them real time like you do (they have uptodate, which I can only assume why it takes 6 hours to admit asthma or whatever.)
Anyways to get back to my points.
1.Keep a close and scrutinizing eye on those VS.
2.And don’t let medicine pretend to be smarter than you.
![Room9er ["Room Niner"]:](https://room9er.com/wp-content/uploads/2020/03/cropped-Screen-Shot-2020-03-08-at-3.16.16-PM.png)