Methemoglobinemia
Background:
- Methemoglobin refers to ferric form of hemoglobin (Fe3+) that is unable to bind O2
- Suspect in any patient with cyanosis not responsive to supplemental O2
Causes:
- Rarely congenital, NADH reductase deficiency – unable to reduce ferric to ferrous iron (Fe3+ → Fe2+)
- Exposure to oxidizing agent
- Benzocaine and other local/topical anesthetics
- Nitrites, nitrates, well water (nitrates)
- Antimalarials
- Quinolones
- Dapsone
- Aniline dyes
- Phenazopyridine
- Sodium nitrite toxicity
Evaluation:
- Oximetry is inaccurate because methemoglobin (MetHb) absorbs light at both 660 nm (red) and 940 nm (infrared) wavelengths approximately equally. This causes the pulse oximeter to fail to distinguish it from oxygenated hemoglobin, resulting in a characteristic, fixed, and falsely low SpO2 reading of around 85%,
- Lack of improvement in oxygen saturation with high-flow oxygen plus discrepancy in oxygen saturation >5% between measurements by ABG vs pulse oximetry (“saturation gap”)
- Diagnosis confirmed by measuring level of methemoglobin in blood
- Normal PaO2
- SpO2 will initially be falsely elevated
- Once MetHb >30% → SpO2 will fall to 80-85%
- Mid-80s SpO2 due to light absorption of both oxyHb and deoxyHb
- “Chocolate brown” color of blood
Management:
- High-Flow Oxygen
- Methylene Blue
- Treat if symptomatic OR asymptomatic with MetHb >25%
- 1-2mg/kg Methylene blue IV over 5min; repeat dose if no effectImprovement seen within 20min
- Contraindicated in G6Pd deficiency (may cause hemolytic anemia)
- Other treatment modalities
- Exchange transfusion for symptomatic methemoglobinemia in patient with G6PD deficiency
- Hyperbaric O2 when methylene blue ineffective or contraindicated
- IV hydration and bicarbonate for metabolic acidosis
Dispo:
- Admit, likely ICU consider Floor if stable
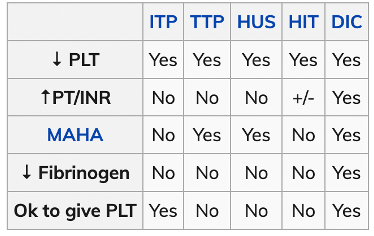
Blood Transfusion Complications
1. Acute Hemolytic Transfusion Reaction (AHTR)
Cause: ABO incompatibility (most dangerous; clerical error)
Pathophysiology:
- IgM-mediated → complement activation → intravascular hemolysis
Presentation (minutes):
- Fever, chills
- Flank/back pain
- Hypotension
- Hemoglobinuria → dark urine
- DIC possible
Labs:
- ↑ LDH, ↑ bilirubin
- ↓ haptoglobin
- Positive direct Coombs
Management:
- STOP transfusion immediately
- Aggressive IV fluids
- Maintain urine output
- Treat DIC if present
2. Febrile Non-Hemolytic Transfusion Reaction (FNHTR)
Cause: Cytokines or recipient antibodies to donor leukocytes
Presentation:
- Fever ± chills
- No hemolysis
Management:
- Stop transfusion (initially to rule out AHTR)
- Antipyretics
- Prevention: leukoreduced blood
3. Allergic Reactions
Mild:
- Urticaria, pruritus
Management:
- Antihistamines → may restart transfusion
Severe (Anaphylaxis):
Cause: IgA deficiency with anti-IgA antibodies
Presentation:
- Hypotension
- Bronchospasm
- Angioedema
Management:
- Epinephrine
- Avoid future IgA-containing products
4. Transfusion-Related Acute Lung Injury (TRALI)
Cause: Donor anti-leukocyte antibodies → neutrophil activation
Timing:
- Within 6 hours
Presentation:
- Acute hypoxia
- Noncardiogenic pulmonary edema
- Bilateral infiltrates
Key distinction:
- Normal BNP
- No volume overload
Management:
- Supportive (oxygen, ventilatory support)
5. Transfusion-Associated Circulatory Overload (TACO)
Cause: Volume overload
Presentation:
- Dyspnea
- Hypertension
- Pulmonary edema
Key distinction from TRALI:
- Elevated BNP
- Signs of fluid overload
Management:
- Diuretics
- Slow transfusion rate
6. Delayed Hemolytic Transfusion Reaction
Cause: IgG antibodies (e.g., Kidd, Duffy)
Timing:
- Days to weeks
Presentation:
- Mild fever
- Anemia
- Jaundice
Management:
- Usually supportive
7. Transfusion-Associated Graft-versus-Host Disease (TA-GVHD)
Cause: Donor T cells attack recipient
Risk:
- Immunocompromised
Presentation (days–weeks):
- Fever
- Rash
- Diarrhea
- Pancytopenia
Prevention:
- Irradiated blood products
Prognosis:
- Often fatal
8. Infectious Complications
Examples:
- Bacterial (platelets highest risk)
- Viral: HIV, Hepatitis B/C (rare now)
Presentation:
- Fever, sepsis
9. Metabolic Complications
Hypocalcemia
- Citrate binds calcium
- → Tetany, arrhythmias
Hyperkalemia
- Stored blood leaks K⁺
Hypothermia
- Large-volume transfusion
![Room9er ["Room Niner"]:](https://room9er.com/wp-content/uploads/2020/03/cropped-Screen-Shot-2020-03-08-at-3.16.16-PM.png)