I will apologize for the wall of text in advance but I thought I to share an experience from last May that fits pretty well with the first 2 weeks of lectures this month. I think it definitely highlights the importance of feeling comfortable with both delivery and newborn resuscitation in case they actually happen to you. I’ve also tried to point out all problems that came about but I am sure I didn’t hit them all and I am positive that I could have handled some of them better.
It was nearly the end of a pretty typical shift at Jewish Downtown. For those of you who haven’t been there or don’t know there is zero OB coverage at Jewish. I was finishing my charts when I hear the secretary say “pregnant woman in labor” over the phone. That is a pretty unusual thing to hear at Jewish so I immediately asked the attending who was sitting closer if I heard that correctly. I also half-jokingly said I definitely wanted in on the patient if they were serious because I still needed a few more deliveries. The attending chuckles and replied that she thought the secretary was only joking because there shouldn’t be any reason for a laboring patient to come to Jewish, so I returned to my charts.
About 2 minutes later they call for a physician from the room behind the doctors area and we walk into what is in fact a laboring patient. The nurses state she seems to be contracting every 3-4 minutes but they don’t know much else at this point. While the attending checks her cervix, I grab the ultrasound and check the fetal position. She was about 8cm dilated and the best I could tell the baby was vertex but the head was so far down I gather this from the rest of the anatomy. Immediately calls start going out to the neonatologist at Kosair while we attempt to talk to the family and figure out how the patient ended up at Jewish. Here comes out first problem:
Problem 1: Neither the patient nor the family speak a word of english. Not only that but there is no translator phone in the room so the family has to be taken to another room to try to get some questions answered.
In the meantime I attempt to get a fetal heart rate to assess how the fetus is doing.
Problem 2: The only doppler is a pen style for checking pulses that doesn’t actually display a pulse number.
I go back to the ultrasound, find the heart and count the beats on the screen while a nurse counts for 15 seconds to get a FHR of about 144, which is always reassuring. In the mean time we are able to obtain some more information from the family.
Apparently, the patient’s water broke during her office visit around 2pm (it’s now almost 11pm) and she was told to go to the hospital. For whatever reason they decided to wait and they got mixed up between Norton’s and Jewish hence our current situation. There are calls being made to Norton’s L&D informing them of the situation and transport is on the way. The neonatologist is also en route as a safety precaution in case she actually delivers here. The patient and fetus appear to be stable, and while still contracting around every 3-4 minutes she still isn’t fully dilated. I make the mistake of leaving the room assuming that the patient will soon be swept away to have her baby properly on an L&D floor. About 5 minutes later another call from the room and I walk in to see the beginning of this baby crowning.
The nurses wheel in their delivery kit as I gown and glove up. I apply a few packets of lubricant jelly, have the nurses move the patient closer to the end of the bed and attempt to create a semi-sterile field with the supplies available.
Problem 3: It’s nice and easy to set up to deliver in a room with a bed designed to deliver a baby. Unfortunately for me this situation involved a nurse/tech on each leg and the patient mostly laying flat in a bed with bag to collect fluid half hanging off the table but mostly just shoved under her bottom as best as I can with no real drainage.
Problems 4 & 5: Did I mention she didn’t speak english, also I have no idea what the word for “push” is in her language. Also when you are on the L&D floor you have all kinds of cool toys such a tocometer to help you know when to tell the patient to push. I do not have that luxury.
I attempt to put a hand on her abdomen to feel her uterus contract so I know when to tell her to push and hope that she figures out what we want from her. Maybe it was a good thought but I have no idea, good thing she does and she is pushing every few minutes and the head is progressing it’s way out.. After a few good pushes the progress seems to slow a little bit and I start to worry a little bit that this 2 week post-dates baby may be stuck. What was that mnemonic for shoulder dystocia again? All I can remember is McRobert’s maneuver, but for anyone curious, Rosen’s has a nice one:
Help: Obstetrics, neonatology, anesthesia
Episiotomy: Generous, possibly even episioproctotomy
Legs flexed: McRoberts’ maneuver
Pressure Suprapubic pressure: shoulder pressure
Enter the vagina: Rubin’s maneuver or Wood’s maneuver
Remove posterior arm Splint, sweep, grasp, and pull to extension
Luckily, I have the nurses holding onto each leg (because this bed doesn’t have stirrups) so they flex her legs towards her as much as they can and everything continues to progress smoothly. Eventually the head is out and the rest of this baby boy delivers quickly. He is suctioned, wrapped in a warm blanket and the nurses begin assessing him. I think we put his APGAR at a 7 at 1 minute.
So I am done right? Baby is out, nothing more to see or do, lets ship them out. Right?……
Turning back to the patient I realize she seems still be bleeding a little more than I expected. It’s hard to figure out where she is bleeding from so I deliver the placenta which appears to be intact. I even sweep and massage the uterus just to be sure which seems to be contracting well.
Problem 6(?): Not really a problem because it seems her bleeding was not coming from the uterus but I have no access to the medications typically used to help control uterine bleeding after a deliver such a pitocin. Not that it matters because I didn’t know what the dose would be anyway. Just another interesting thought that I had during this whole process.
Since the placenta is whole, and seems to be firm I look for other sources of bleeding. This is when I realize the patient has a nice 2nd or 3rd degree tear (Dr Sterrett would be very disappointed I didn’t control the head well enough). I check to make sure it isn’t a 4th (thankfully it’s not), and start contemplating my next course of action. The attending asks what kind of suture I want to use to repair her tear. My only reaction was to smile and say “nothing”, followed by explaining that since the bleeding is slowing it’d probably be better to let the OB-GYNs fix her. I plan to pack her to make sure she doesn’t bleed too much in transport.
Problem 7: No one had even seen a vaginal packing kit in the ED before, so we improvised and used some kerlex with a tail for easy removal.
By the time this had finished the neonatologist had arrived and began assessing the newborn. I think we ended up giving him apgars of 7 and 9. I started the patient on some fluids (because we didn’t have an IV when all of this started, another mistake I didn’t realize until it was all over) and within another 2 minutes transport had arrived to take the patient to Norton’s and she was actually swept away. Hopefully the OBs she finally got to didn’t think I botch the whole thing too much. Overall it was a pretty intimidating and adrenaline pumping situation. Not sure if I will ever have an experience quite like this again but if it does happen at least it will not be the first.
Any comments, critiques, criticism or otherwise are welcome.
![Room9er ["Room Niner"]:](https://room9er.com/wp-content/uploads/2020/03/cropped-Screen-Shot-2020-03-08-at-3.16.16-PM.png)
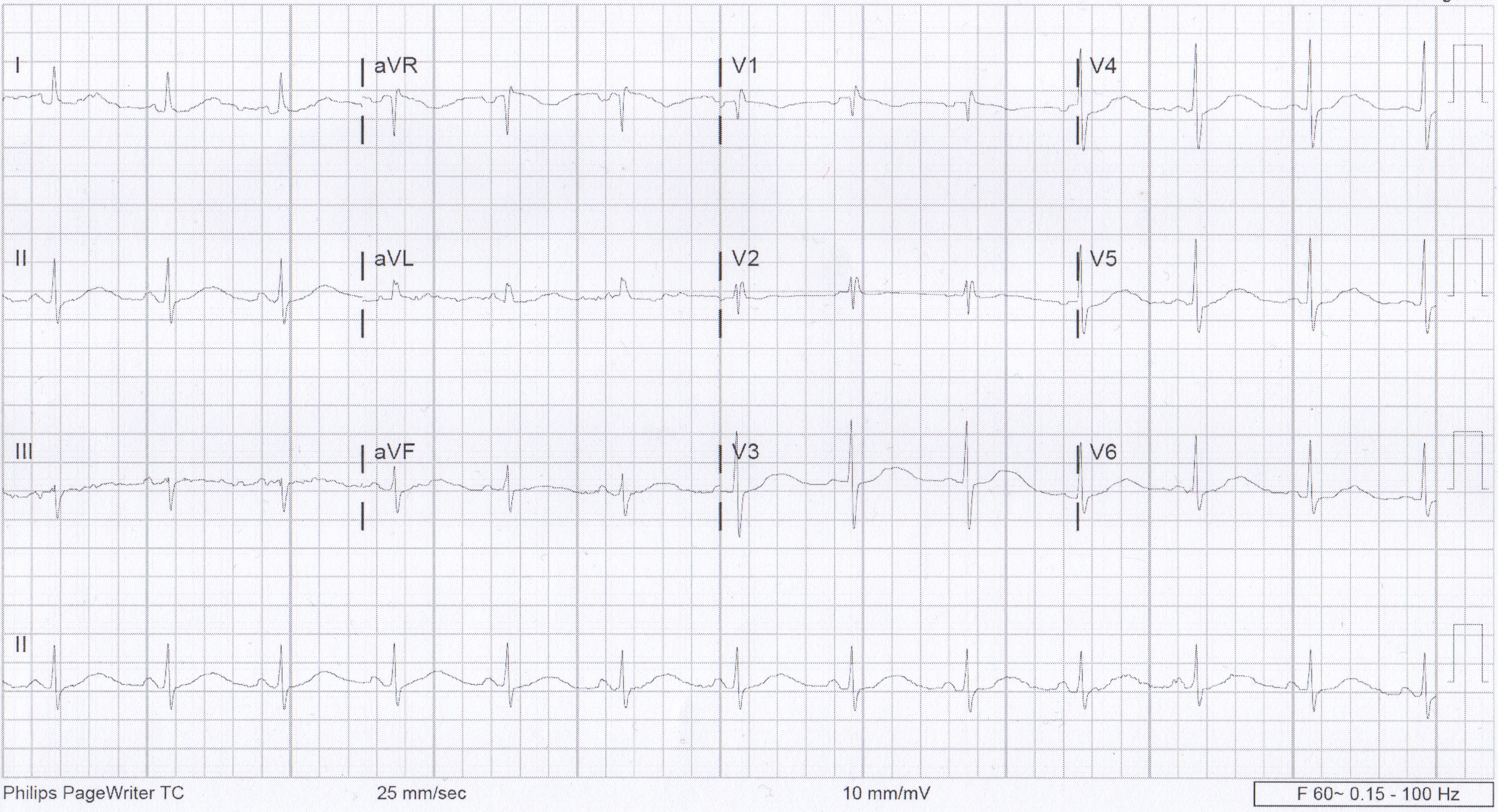
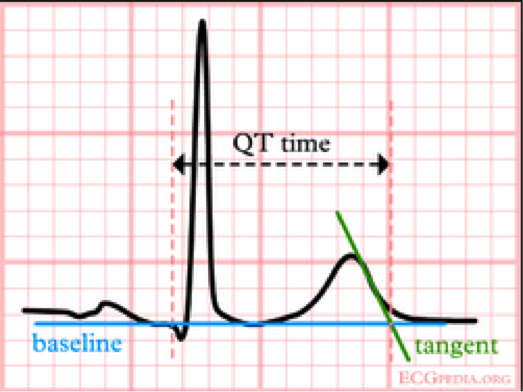
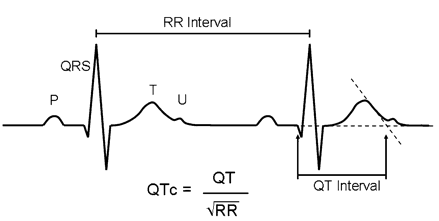 We usually talk about QTc rather than just the QT. This is because the QT interval varies depending on the HR. Using a correction equation standardizes the interval so it can be interpreted regardless of the HR. The EKG computer does give a calculation of the QTc, because we are obviously not hand calculating this on every patient. You should compare what the computer calculates to your gestalt when you review the EKG. If there are any concerns or discrepancies, you should hand calculate the QTc.
We usually talk about QTc rather than just the QT. This is because the QT interval varies depending on the HR. Using a correction equation standardizes the interval so it can be interpreted regardless of the HR. The EKG computer does give a calculation of the QTc, because we are obviously not hand calculating this on every patient. You should compare what the computer calculates to your gestalt when you review the EKG. If there are any concerns or discrepancies, you should hand calculate the QTc.