McGowan – Teaching series
Scaffolding –
- Establish a baseline (Know your audience)
- Cues
- Leading qs vs reflective
- Breakdown tasks
Ex )
- SOAP notes
- ACGME milestones
- Certifying exam checklist
- Procedural skill learning
- Sim
- OSCE
- SLOE
- Consider graphic organizers for ddx
- Gridded Charts
- Flow charts
- Worksheets
Final thoughts
- Assess learners baseline
- Adjust level of intervention based on thiss
- Have clear objectives
- Short and sweet
- break down to smaller tasks
- Foster safe environment
- Failing is ok if you learn from it
Coffman – Question
Kelesis – RM9 Follow Up
27 F w ho asthma, prior suicide attempt presents after unknown but large ingestion ibuprofen
- 5 large bottles 200mg ibuprofen empty
VBG 7.3/33.5/82/-9.5
CHEM8 139/3.6/108/143/1.14
Lactic 5.0
Intubated for aspiration risk w prop fent
CXR ok
CT head ok
C/f for lactic acidosis (AGMA), bleed, kidney injury
Rpt gas w ph 7.1, lactic to 8.3, Gap 19
HD placed, admitted to MICU underwent HD, still admitted to 3N
Reversible binding COX1/2 -> depletion of thromboxane = bleed
Peak plasma concentration 1-2hrs
Activated charcoal within 2 hrs of ingestion can be considered
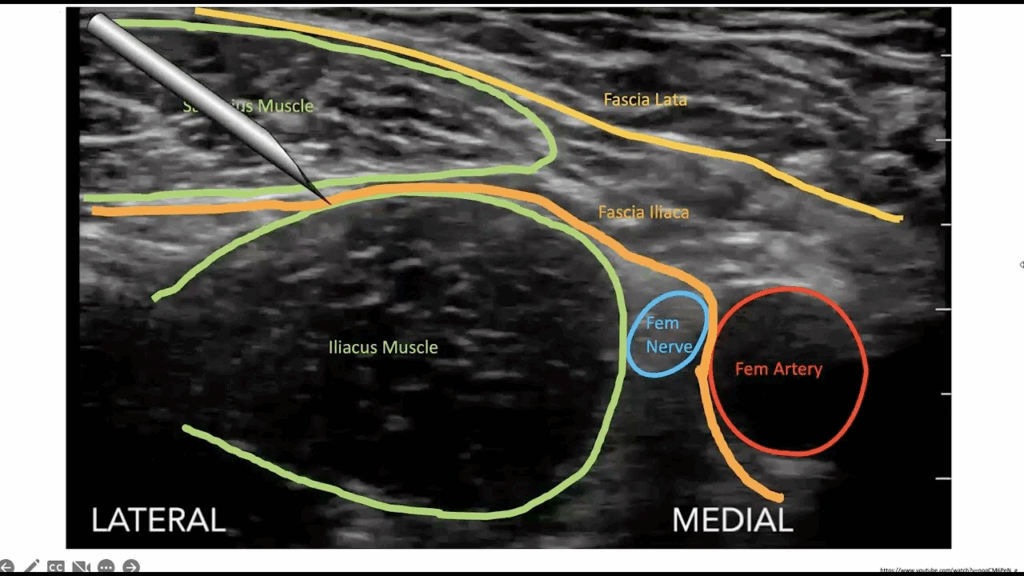
Davenport – Shock US
I – indications
A – acquisition
I – interpretation
M – MDM
Pump – heart squeeze, beating, effusion
Pipe – IVC – plump, collapsable
Problem
Cardiogenic shock
- LV dysfunction w PLAX, PSAX
- IVC – plethoric
- EPSS on PLAX
- Line on mitral valve
- Measure peak of valve to septum
- >7 = poor LVEF
- Lungs
- Needs to be 15cm to be considered B line
- Consider turning off tissue harmonics for brighter B line
- 3 B lines per view for dx
Obstructive
- Tamponade
- Speed of accumulation important
- Mitral valve inflow integral
- Doppler at mitral valve outflow on A4C
- Measure tallest expiration wave to lowest expiration wave
- >25% = pulsus paradoxus
- Plethoric IVC
- PE
- D sign on PSAX, bc higher pressure in R heart
- Mcconnel sign on A4C, bc RV free wall hypokinetic
- Tricuspid annular plane systolic excursion
- M node on A4C on tricuspid
- Measure peak to valley <16-17 = acute heart strain
- M node on A4C on tricuspid
- Tension ptx
- Plethoric ivc
- Heart could be hyperdynamic, flattening of R heart
- Lung slide
- Can mmode for barcode sign
- US more sensitive than CXR
- Lung point
Hypovolemic
- Hyperdynamic echo
- FAST
- Aorta – measure outer to outer, anterior to anterior
Distributive
- Hyperdynamic echo
- Flat IVC
- RUQ
- Pericholecystic fluid
- Anterior wall thickening in short access
- <3mm normal
- Sonographic murpheys
- CBD
- Measure inner to inner
VEXUS (on icu pts s/p open heart sx)
- Measurement on venous congestion
- Organ perfusion pressure
- Determine modality of tx
- Prevent AKI, HF, pulm edema, poor wound healing
IVC widest diameter in subcostal view, >2cm moveone, less thant 2 = noncongestion
Hepatic vein w indicator towards pt head, find vein entering IVC
- Doppler
Portal vein w indicator towards back
- Doppler
Renal vein
Compare waveforms and grade
- High grade = diuretics
Obrien – Pituitary
Sheehan – pituitary grows in pregnancy but not blood supply, vulnerable to hypotension
- Tx w hydrocortisone
Pituitary apoplexy
- Tx w hydrocortisone to address ACTH deficiency
Acromegaly – excess GH from pituitary adenoma
- Dx w serum insulin like growth factor level
SIADH –
- Tx hypona sz with hypertonic, consider amps of bicarb
- Aim to correct 4-6 meq/L
- Beware of cerebral edema
- Avoid isotonic fluids – makes them worse cause they hold onto free water
Congenital hypopituitary
- Hypoglycemia, sex organ weirdness, jaundice, midline deficits
- Tx glucose and hydrocortisone
Optic chiasma – pituitary masses compress this
- Bitemporal hemianopsia
- Little = endocrine issues
- Big = mass effect
Prolactinoma – most common pituitary tumor
- Tx cabergoline to inhibit prolactin release
![Room9er ["Room Niner"]:](https://room9er.com/wp-content/uploads/2020/03/cropped-Screen-Shot-2020-03-08-at-3.16.16-PM.png)