Alternatives to Labetalol- Drug currently on Shortage
Author Archives: Adam Ross
EM Cases: Occult Knee Injuries
Good 5-10 minute read with lots of pearls on Knee Injuries in the ED, their assessment, exam findings, and management.
Decreased Survival with Intubation During Cardiac Arrest
Quick Read on something I feel like comes up a lot with our cardiac arrest patients. They don’t typically need intubated, they need good CPR. Bag or put an LMA in and stop at that. While the numbers aren’t astounding, given the differences in such a large amount of patients think these make sense.
http://www.healio.com/cardiology/arrhythmia-disorders/news/online/%7B5396b1a2-0167-4a2d-885c-0e1bc527398e%7D/findings-do-not-support-early-tracheal-intubation-for-in-hospital-cardiac-arrest-in-adults
Top Ten UTI Myths
Good 5-10 minute read on myths regarding UTI and asymptomatic bacteriuria. Hope you’ll take a look as this is a common problem in many EDs, not just ours with regards to over-diagnosis and over-treatment.
http://www.medscape.com/viewarticle/865175
Ross
Level 1 Rapid Infuser & Autotransfusion
All,
Couple videos on what was covered today with Level 1 Infuser and Autotransfusion. They’re not bad, definitely get the overall setup at least. With the autotransfusion videos, there are a few small differences in their setup vs ours I think, but overall for your purposes is mostly the same. Hope this helps.
Ross
Level 1 Infuser
https://www.youtube.com/watch?v=9YIROsYE_Yo
Autotransfusion
https://www.youtube.com/watch?v=WmLs-43jaR4
Good read on HEART Score
Central Line Insertion Choice
All,
I know this came up during conference today so thought I’d send the article I think was cited. At least this is the one I found from EMRAP, below is their summary of this article. Long and short of it, complication rates are really low, when done in sterile fashion in a controlled environment.
This was done in the ICU, not in the emergency department.
Overall they didn’t say that one site was absolutely the best.
nejm-2015-central-line-site-complications
Take Home Points
No central line site is superior.
Femoral lines are fastest and most successful. Subclavian lines have a lower infection risk but higher rate of pneumothorax.
Parienti, JJ et al. Intravascular complications of central venous catheterization by insertion site. N Engl J Med. 2015 Sep 24;373(13):1220-9. PMID: 26398070
Bottom line: no line was superior. Femoral lines were the fastest to place and had the highest success rates. Subclavian lines had the lowest infection risk but had a higher rate of pneumothorax.
A patient needs central line access. Which should we choose? Which is best? There are multiple complications; infection, mechanical complications like artery puncture or pneumothorax and thrombotic complications.
The authors of this study conducted a randomized, controlled trial in 10 French ICUs. They enrolled adult patients with at least two accessible sites. Patients with all three sites accessible were randomized in a 1:1:1 fashion while those with only two sites were randomized in a 1:1 fashion. The doctors had all performed at least fifty central lines. However, they were all aware of the study and probably tried harder to reduce complications.
They looked for symptomatic clots and/or infection from the time of insertion up to 48 hours after removal. This was a large study; 3471 catheters were placed in 3027 patients. Catheters were assigned to a randomly assigned site and side; placement was successful approximately 91% of the time. 85% of subclavian lines were successfully placed, 91% of the jugular lines were placed and 95% of the femoral lines were placed. Femoral lines were most successful and subclavian lines were least likely successful.
Placement of femoral lines was also more rapid, by about a minute.
The primary outcome was a composite of infection, symptomatic clot and mechanical complications such as pneumothorax and bladder puncture. The jugular line performed the worst followed by the femoral line, then subclavian line. However, it is important to look at the individual components.
For mechanical complications, the subclavian line performed the worse. 2% had a complication versus 1.5% of jugular lines and less than 1% of femoral lines.
All lines were fairly low for symptomatic clots; 0.5% for subclavian, 1% for jugular and 1.4% for the femoral group.
In terms of infection, the subclavian group was the lowest (0.5%). The highest? Surprisingly, jugular lines had a 1.4% rate of infection versus 1.2% in the femoral line group.
Overall, there were fairly low rates of complications. These were performed in very sterile conditions in the ICU. These were not placements in crashing or coding ED patients.
Placement of central lines, including femoral lines, when done carefully under sterile conditions has a low rate of complications. This article does not identify one superior line placement.
Gram Negative Coverage
Quick 2-3 minute read on gram negative coverage @ ULH (brought to you by my wife, the ID pharmacist). Less resistance with Tobramycin than with Levaquin.
Potential Management Change in Uncomplicated Diverticulitis
I had read a different article recently talking about the AGAs recommendation change regarding uncomplicated diverticulitis; here’s another one from ACEP Now citing similar data. Perhaps another condition we can stop writing unnecessary antibiotics for. Do keep in mind this is for UNCOMPLICATED cases.
Routine Coags in Chest Pain
Thought this was a great little post regarding Coagulation studies in chest pain patients. Not sure how often its getting routinely obtained on our CP patients @ UofL but at Norton they get it on almost every chest pain patient that rolls through the door.
We’ve reduced the amount of coag studies we’re getting on our routine trauma patients, probably about time we make sure we’re doing the same in our low-risk chest pain patients.
The Hypercoagulable Liver Failure Patient?
Hey Guys,
Just listened to a portion of April EM:RAP (so if you’ve heard it already here’s a little repetition) and was surprised to hear their Notes from the Community Section about coagulopathy in Liver Disease, which basically informed me that many liver patients are at just a high of risk of thrombosis as they are of bleeding.
3 Articles were referenced:
– Tripodi A, Mannucci PM. The coagulopathy of chronic
liver disease. N Engl J Med. 2011 Jul 14;365(2):147-56.
– Villanueva C et al. Transfusion strategies for acute upper gastrointestinal bleeding. N Engl J Med. 2013 Jan 3;368(1):11-21.
– DeLoughery TG et al. Invasive line placement in critically ill patients: do hemostatic defects matter? Transfusion. 1996 Sep;36(9):827-31.
Summary:
– The liver makes both procoagulant and anti-coagulant proteins which can be actually reduced close to equally rendering the patient basically in equilibrium (thus not so hypercoagulable).
– No study has shown that coagulation defects predict issues with procedures (but the experience of the clinician performing the procedure does).
– INR is not standardized in Liver Failure patients (like it is with Warfarin) and thus is not that helpful.
– PT & PTT may also not be helpful in patients with liver failure (due to the variability of loss of clotting factors)
**Fibrinogen may be low in liver failure patients, and you may consider replacement of this with Cryoprecipitate (10 units of Cryo increases the Fibrinogen by 100mg/dl).
– Raising intravascular volume with pRBCs may make them bleed more.
For the full references & discussion see the EM:RAP written summary. Perhaps this is something we should discuss with our GI colleagues and/or MICU people. Any thoughts?
March EM:RAP Summary
Hey Guys,
Just some things I learned on EM:RAP this month, and since I’m on admin thought I would post a few things.
The DRE (not the rapper Dr. Dre): from the Fingers & Foley’s section on EM:RAP; reviewed Esposito TJ et al. Reasons to omit digital rectal exam in trauma patients: no fingers, no rectum, no useful additional information. J Trauma. 2005. They had 512 trauma patients at a Level I Trauma Center. “the negative predictive value of both the rectal exam and other clinical indicators was very high: 99%. However if the other clinical indicators missed the injury, so did the rectal exam. It didn’t add any information”
Basically showed added value of a rectal exam to be very minimal, and that ROUTINE RECTAL EXAM IS NOT RECOMMENDED. BTW, this is in the journal of trauma which is well-regarded amongst our surgery friends.
How to identify if patient’s contact lens is still in the eye (e.g. if patient has eye pain and feels like its still in there and can’t find it): Use Fluorescein much like you would for corneal abrasion as it will stain the contact lens as well, allowing you to find it (then you can evaluate for corneal abrasion at the same time). *keep in mind contact lens will be ruined*
Subarachnoid Hemorrhage: from an article in JAMA in Sept 2013 with 10 university affiliated Canadian EDs. Tried to come up with a decision rule for SAH and basically came up with:
The decision rule including any of age 40 years or older, neck pain or stiffness, witnessed loss of consciousness, or onset during exertion had 98.5% (95% CI, 94.6%-99.6%) sensitivity and 27.5% (95% CI, 25.6%-29.5%) specificity for SAH. Adding “thunderclap headache” (ie, instantly peaking pain) and “limited neck flexion on examination” resulted in the Ottawa SAH Rule, with 100% (95% CI, 97.2%-100.0%) sensitivity and 15.3% (95% CI, 13.8%-16.9%) specificity.
**Key points: this decision rule is more to identify high risk patients and the high risk symptoms. Sensitivity was very high, but specificity very low. Also keep in mind there are other important causes of headache to keep in mind**
Biphasic Reactions in Anaphylaxis: from Annals of Emergency Medicine in November 2013. A chart review was performed over 5 years and had ~500 pts with anaphylaxis, but also documented allergic reactions. Found biphasic reaction was extremely rare (2 cases while in the ED, and 3 out of the ED), with a rate of 0.4% while in the ED. 6% bouncebacks in the anaphylaxis group, none of which died and none of which came back in anaphylaxis. This study was limited in that it was retrospective, and there was variability in the outpatient management of these patients (unclear who was DC’d with what if any medications)
Rosen’s states corticosteroids can be helpful in reducing risks of protracted anaphylactic reaction and biphasic anaphylaxis (7-10 day course). H1 & H2 antihistamines are helpful in reducing some of the symptoms of anaphylaxis. 5-Minute Emerg Consult recommends Epi-Pen for those with anaphylaxis.
No Formal observation time has been established, though Rosen’s says 2-6 hours; with longer observation times/admission for those with prolonged reaction or requiring multiple dose epinephrine
Sorry this is so long, but I’m on Admin so thought I’d post something. Attached you’ll find the March Written Summary with all the articles they referenced. Hope this is helpful.
Utility of a CXR
Hey Guys,
Thought I’d post this as I feel it was a mistake on my part, though fortunately no harm came from it.
50 year old guy this past Saturday (which was a ridiculous shift full of drunks and unhelmeted mopeds and motorcyclists with some very sick people) who was an unhelmeted moped rider going reportedly 60mph and wrecked while drinking alcohol and somehow managed not to make their way to Rm 9.
BP: 125/73. HR: 86. RR: 18. O2 saturation: 91% on room air. Temp: 97.6 F (oral)
A&Ox3, c/o shortness of breath and diffuse chest tenderness. Not really any obvious bad looking signs of trauma and had been log-rolled prior to my eval (triaged about 1hr 45min before I saw him).
I saw him, in no respiratory distress, maybe some expiratory wheezing on my exam, but with breath sounds on both sides and no crepitus that I could feel to his anterior chest. I finish my eval and just order a MAN scan based on his Hx and due to his drinking alcohol (EtOh 292)
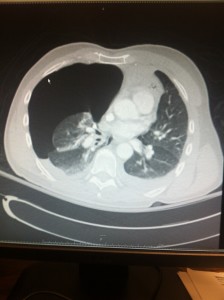
Patient is taken to CT at 23:05 (about 2 hrs after I ordered them) and the nurse grabs me after the scan and tells me I need to look at his chest CT (only his C-spine images were up at the time which showed me all kinds of SubQ emphysema).
Just a lesson learned; when it’s super busy like that shift was is when we need to be the most cautious and really think critically about the things we need to do, and not be in a hurry when we’re putting orders in.
The guy is doing well so far (and not intubated) and in THIS case no harm was done, I put a chest tube in without difficulty. But I really should have gotten a CXR to start.
His injuries included Bilateral 1st-6th Rib Fx’s, Pulmonary Contusions, Mediastinal Hematoma, Manubrium Fx, C7 Fx, T4, T7 Fx.
![Room9er ["Room Niner"]:](https://room9er.com/wp-content/uploads/2020/03/cropped-Screen-Shot-2020-03-08-at-3.16.16-PM.png)