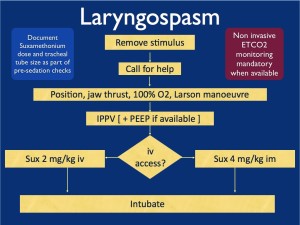
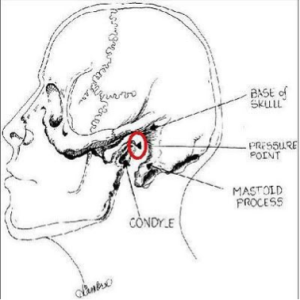
I had a case of epistaxis the other day so I thought it would be interesting to review the management here. All of the following information can be found in Tintinalli’s, and there are also some great instructions in Roberts and Hedges. Disclaimer: this is not a complete review of epistaxis, mostly just the management. You can review the pathophysiology/epidemiology/important historical aspects/etc in your reference of choice. Here we go:
The management starts with a good physical exam. You need to figure out whether this is an anterior or posterior bleed. Posterior bleeds are much rarer, but are more difficult to control and usually bleed a lot more and require ENT assistance. The right equipment is essential.
Find a mask with a shield, a good light source, a nasal speculum, some 2×2 gauze, and some bayonet forceps. Position the patient upright and have them blow all the clots out of their nose (you might want to step back for this part). Using your equipment you’ve already laid out, look into the nose to see if you can identify the bleeding. Most cases are anterior bleeds, so you will likely see the source of bleeding (usually Kiesselbach plexus in the anterior septum). Spray some oxymetazoline or phenylephrine in the affected naris (or both if it’s not clear) to constrict the vessels. Now it’s time for direct pressure. Some hospitals have commercial devices that will do the work for you. If not, you can tape 2 tongue depressors together starting from one end and going about halfway, leaving the other end open. This can then be used to pinch the patient’s nose closed. Leave undisturbed for 15 minutes…..
Congratulations! You’ve just put a stop to most cases of epistaxis. If you’re not that lucky, it’s time to escalate. If you’ve identified the source of bleeding, you can try silver nitrate. Provide analgesia by soaking your gauze in a 1:1 mix of your vasoconstrictor and 4% Lidocaine and placing it in the anterior nose for a few minutes. Then, go back and cauterize with the silver nitrate. Avoid more than 3 attempts, and never cauterize both sides of the septum.
Still bleeding? Well, nevermind that busy ED you’re running, or the multiple ambulance crews dropping off more patients. Time to try a last ditch move before packing. You can try Gelfoam or Surgicel, or you can also try soaking some gauze in TXA and applying pressure over the site of bleeding with that. But if the patient continues to bleed, it’s probably time to pack…
Anterior nose packing can be done in multiple ways. Many EDs have the Rhino Rocket, or some other form of anterior nasal balloon. You insert these along the floor of the nasal cavity, and gently inflate with air (don’t use saline in case it ruptures). Other types of anterior packs have a sponge material which will expand inside the nose once it contacts the blood. You can also add a few mLs of saline to help it along. If the bleeding continues, you may try anterior packing the other naris. If you are unfortunate and work in an ED that does not have these devices, you will need to use strip gauze to fashion your own pack (again, great pictures in the references mentioned above).
If you’re still bleeding, it’s probably time to call for help. Continued bleeding despite the above measures suggests a posterior bleed. You can perform a posterior nasal pack while waiting for your specialist, or if you do not have ENT available. There are more commercial devices available that are longer and have an additional balloon for posterior packing. If you don’t have this available, you can use a 14 French foley catheter. Anesthetize the nose once again as before. Cut off the distal end of the foley past the balloon. Lubricate the end with Lidocaine gel, and advance along the floor of the nasal cavity, continuing until you can see it in the oropharynx. Now inflate the balloon with 7 mL of air, and retract a few centimeters to lodge it in the posterior nasopharynx.
Dispo: If anterior bleeding has been controlled, patient may be discharged with ENT followup. If packing is in place, antibiotics are controversial. Consider starting Augmentin to cover for Staph aureus and toxic shock syndrome. Posterior packs need to be admitted for further management by ENT.
Solid work! There are only 6 new ones to pick up…..
![Room9er ["Room Niner"]:](https://room9er.com/wp-content/uploads/2020/03/cropped-Screen-Shot-2020-03-08-at-3.16.16-PM.png)