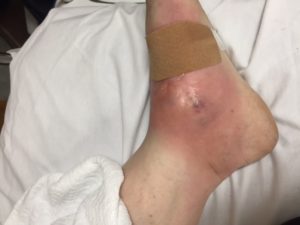
55 y/o F with hx of HTN,COPD and recurrent indurative lesion on her left foot, last event was a yr or so ago, presented to the ED for worsening pain and increased size of her lesion for the last few wks now. No fever, chills, or fatigue. On exam, the cutaneous lesion is mildly tender and erythematous, non-fluctuant, no warmth noted. Pt is immunocompetent.
/
/
/
/
/
/
/
/
/
/
/
/
Answer:
Pyoderma Gangrenosum. Take home point is to not I&D this lesion. It is not an abscess. It is a rare autoimmune disease that affects pts in their 40s-50s. These pts will have hx of other autoimmune diseases–lupus, crohns etc. An I&D would lead to phenomenon known as pathergy, the formation of new lesions following a trauma.
Tx: High dose steroids and pain meds. Refer to podiatry. Pt in this case was already well known to podiatry on arrival and was discharged with steroids and pain meds after podiatry consult in the ED.
![Room9er ["Room Niner"]:](https://room9er.com/wp-content/uploads/2020/03/cropped-Screen-Shot-2020-03-08-at-3.16.16-PM.png)