A late 20s F G4P3003 at approximately 6 weeks gestation by LMP presents with a chief complaint of vaginal bleeding. A few hours PTA, patient states she felt a “gush of blood” with some mild abdominal cramping. VSS. On exam, noted to have a moderate amount of vaginal bleeding per the os. On our bedside ultrasound we note what appears to be a viable IUP with cardiac activity. However, the uterus appears septate, with half containing the IUP and the other half more hyperechoic/solid in nature. We were concerned for a possible subchorionic hemorrhage and consulted OB/GYN. Our bedside US image is below:
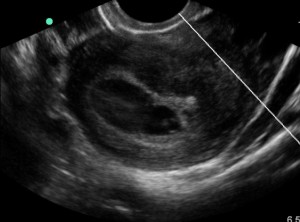
OB came down with their Cadillac ultrasound and confirmed our findings. For comparison, here is their much clearer image:
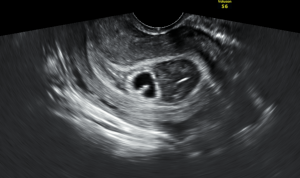
For this patient, with this large of a subchorionic bleed, the likelihood of her carrying this pregnancy to term was low. They planned to have her follow up in clinic for a repeat ultrasound in 2 weeks to reassess viability. Per our OB colleagues, other things on the differential included a fibroid. However, as this patient had 3 very healthy and rambunctious boys at the bedside with her, OB commented that a fibroid that large would likely have resulted in infertility.
And from UptoDate:
“A subchorionic hemorrhage or hematoma is a risk factor for spontaneous abortion, particularly when it amounts to 25 percent or more of the volume of the gestational sac. A meta-analysis of seven comparative studies found that women having a subchorionic hematoma had a significantly increased risk of spontaneous abortion, compared to women without such findings (18 versus 9 percent; OR 2.18, 95% CI 1.29–3.68). The findings also are associated with an increased risk of placental abruption (4 versus 1 percent; OR 5.71, 95% CI 3.91–8.33) and preterm premature rupture of membranes (4 versus 2 percent; OR 1.64, 95% CI 1.22–2.21). The increased risks of preterm labor and stillbirth appeared to be dependent upon the presence of vaginal bleeding.
Pregnancy outcome associated with subchorionic hematoma also relates to location, with worse outcomes observed for retroplacental hematomas, compared to marginal hematomas. The location, rather than the size, of a subchorionic hematoma may be the most important predictor of pregnancy outcome. Evidence relating to the size of the hematoma and the risk of adverse outcomes is inconclusive.
The only management option for subchorionic hematoma is expectant. There is insufficient evidence regarding whether bed rest decreases the risk of pregnancy loss when a subchorionic hematoma is present. Some clinicians repeat an ultrasound in one to two weeks to confirm fetal viability and assess any change in size of the hematoma, primarily to provide reassurance to the patient. A subchorionic hematoma is not an indication to conduct a diagnostic evaluation for an acquired or inherited thrombophilia.”
![Room9er ["Room Niner"]:](https://room9er.com/wp-content/uploads/2020/03/cropped-Screen-Shot-2020-03-08-at-3.16.16-PM.png)