Middle age male brought into Room 9 s/p crush injury. The patient was reportedly crushed against a box truck and a wall for a short period, but no prolonged extrication.
He complains of LUQ chest pain, pleuritic in nature, and denies abdominal pain. He was ambulatory after the event. PMH only significant for HTN, otherwise no PSH, no allergies, and takes lisinopril and hydrochlorothiazide.
He is AOx3, moving all extremities, well appearing in Room 9, and acting appropriate. He goes for man scan as he did strike his head and although can give me all the details of the accident he reports LOC.
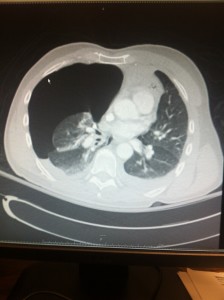
Upon return from the CT scanner his VS are stable, and is placed in a regular ED bed. Image review revealed multiple rib fractures, and suspicious appearing spleen. Radiologist confirms grade 1 spleen laceration, but no active extravasation, as well as bilateral rib fractures.
While evaluating another Room 9 patient, the nurse came to update me that the patient was now unresponsive and foaming at the mouth. I told her to give Narcan, thinking it could be iatrogenic analgesia toxicity, and I would be right there.
I arrive in the room, and he does NOT look right. He is foaming at the mouth, the narcan certainly changed his pupil size when she gave it, but did nothing to his mental status. Sternal rub, nipple pinch, and ammonia capsule all failed to appropriately arouse him. The trauma resident is now at the bedside as well and just as perplexed as this isn’t what I described on the phone. I call radiology ask them to re-check his CT head but they said no, they see nothing. I again re evaluate him and now he will move only his L side, and follow commands on the L side of his body.
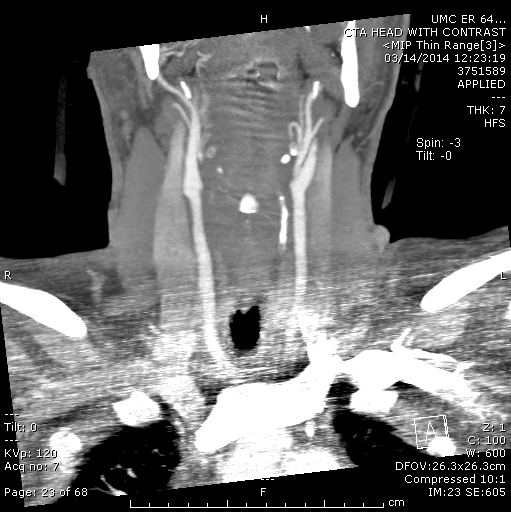
Well…..crap, this is dysarthria R sided hemiplegia. Stroke paged, obtained stat CTA head and neck, and then straight to Room 9 to intubate him. See the CTA imaging below:
Carotid artery dissection…
He obviously is not a tPA candidate, but he did go for an intervention procedure with the stroke service. He did have a clot retrieved, but I have visited him on the floor a few days later and he had no improvement.
He went on to develop cerebral edema as well and had a large hemicraniectomy. He also had an ex-lap for an increase in abdominal distension, and found to have pancreatic ascites (3L removed from the abdomen). The spleen did fine.
Looking back, his mechanism did not support a reason for him to dissect a carotid. He had no external signs of injury, he had no neck pain, my guess is he did have a whiplash type injury but again, not something I expected. In addition, this man had a normal neuro exam upon presentation, full strength, no numbness/tingling with the exception of reporting headache, which I thought was from him striking his head.
After a lit review, there are a few teaching points I want to highlight from this case.
Traumatic Dissection (carotid, vertebral, spinal arteries)
– consider it with hangings, significant head/neck trauma, hyper-extension injuries, lateral rotation injuries of the head, base of the skull fx, c-spine fractures(especially those with displacement or involvement of the transverse foramen,vertebral body), lefort fractures (types II and III), or seat-belt sign over the neck
– Sign/Symptoms vary greatly. Stroke like symptoms are concerning but can be as generalized as headache/migraine, neck pain, neck hematoma, blindness, aphasia, weakness/sensory loss, Horner’s syndrome, tinnitus, CN deficits, diplopia, locked in syndrome, ataxia, vertigo, dizziness
![Room9er ["Room Niner"]:](https://room9er.com/wp-content/uploads/2020/03/cropped-Screen-Shot-2020-03-08-at-3.16.16-PM.png)